Spider Veins vs Varicose Veins: Key Differences
Many people notice visible veins on their legs and wonder whether they are spider veins or varicose veins. These two conditions share some similarities, but they are not the same. Understanding the key differences helps people recognise what’s normal, when to seek a medical assessment, and what treatments may be suitable for their situation.
This guide explains what each condition looks like, how they form, why they develop, and how our doctors assess them.
What are Spider Veins
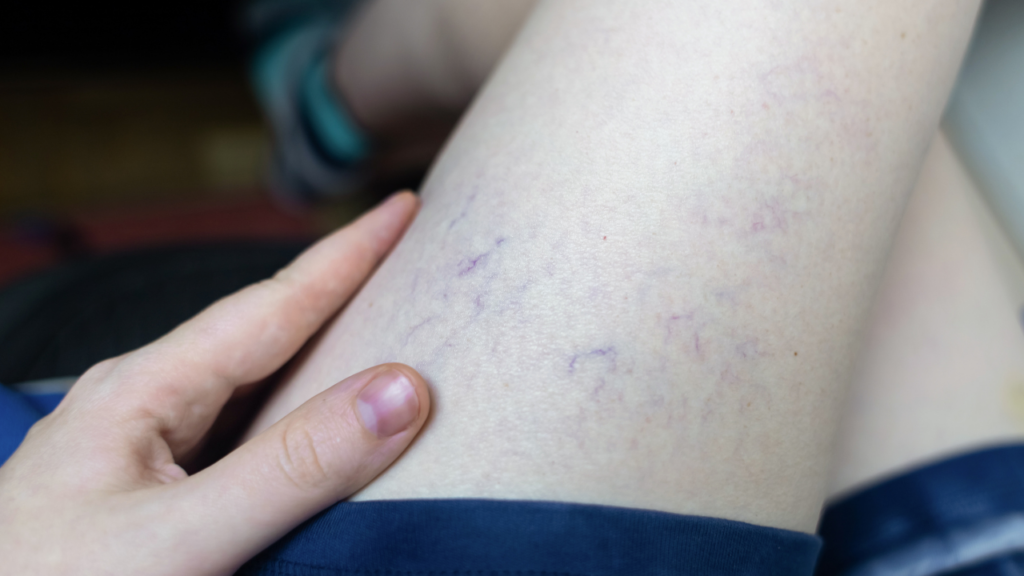
Spider veins are very small surface veins, usually less than 1 mm in diameter. They often appear as thin red, blue or purple lines close to the skin. Many describe them as “web-like” or “thread-like” clusters.
They most commonly form on the thighs, ankles and calves, and can appear on the face. While spider veins can be a cosmetic concern, they may also occur alongside deeper vein issues. A proper assessment helps determine whether they are isolated or linked to underlying venous insufficiency.
What are Varicose Veins
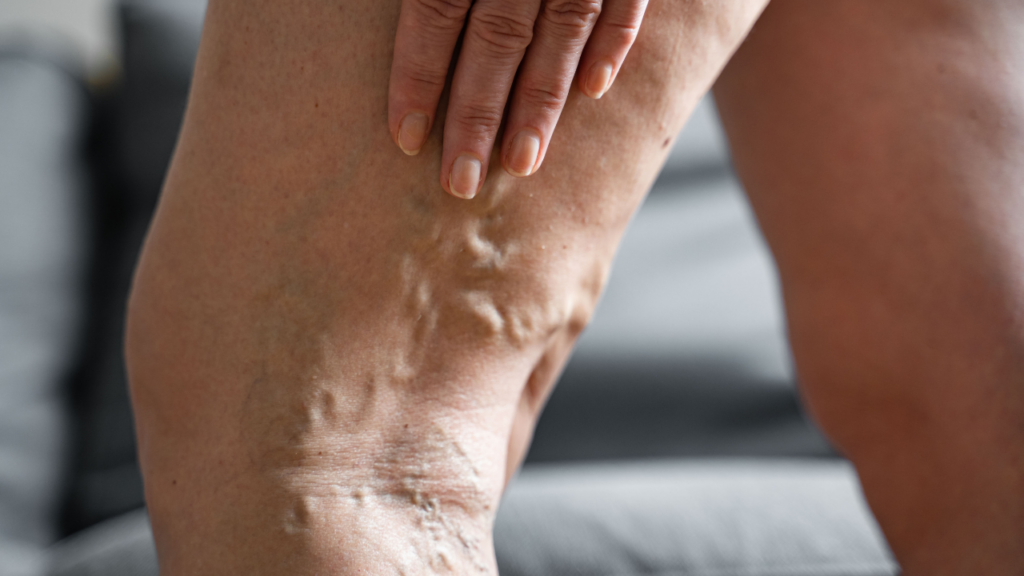
Varicose veins are larger, swollen, twisted veins that sit deeper under the skin. They often appear raised, rope-like or bulging. Varicose veins develop when the valves inside the veins stop working efficiently, leading to pooling of blood and increased pressure.
Patients in Brisbane and the Gold Coast often notice varicose veins after long periods of standing, during pregnancy, or as part of a family history of vein conditions. Symptoms can include heaviness, aching, swelling or discomfort, particularly at the end of the day.
Spider Veins Vs Varicose Veins: Key Differences
While spider veins and varicose veins can appear together, they are two separate conditions. The table below highlights the main distinctions.
Feature | Spider Veins | Varicose Veins |
Appearance | Small, flat, colourful lines | Large, bulging, twisted veins |
Size | <1 mm | 3 mm or larger |
Depth | Surface level | Deeper veins |
Common Symptoms | Often none, may cause mild discomfort | Heaviness, aching, swelling, throbbing |
Cause | Capillary dilation, hormonal or genetic factors | Valve dysfunction leading to venous insufficiency |
Assessment | Visual examination | Ultrasound assessment |
Having both conditions is very common. Spider veins may be visible on the skin while deeper varicose veins are present underneath.
What Causes These Vein Conditions
Both spider veins and varicose veins develop due to changes in how blood flows through the veins. While they may look different on the surface, they often share similar contributing factors.
Understanding the cause is important because treatment should always address the underlying issue, not just the visible veins.
Shared Risk Factors
Both spider veins and varicose veins may share similar contributors, such as:
- Genetics or family history
- Hormonal changes
- Pregnancy
- Ageing
- Prolonged standing or sitting
- Previous injury to the legs
- Lifestyle factors
The Underlying Mechanism Is Different
Although spider veins and varicose veins share risk factors, the mechanism behind them differs.
Learn more about underlying vein issues on our Varicose Veins page or explore Australian Ultrasound Specialists to understand how ultrasound is used in the diagnosis process.
Spider Veins: Surface Vessel Dilation
Spider veins usually result from dilation of very small superficial vessels near the skin surface (called telangiectasia). These fine veins widen and become visible as red, blue or purple lines.
In many cases, spider veins are isolated to the surface. However, sometimes they may be associated with deeper venous reflux. This is why clinical assessment — and in some cases duplex ultrasound — is important before treatment.
Treating surface veins alone without assessing underlying flow can lead to incomplete results or recurrence.
Varicose Veins: Valve Dysfunction and Venous Reflux
Varicose veins develop when the one-way valves inside larger veins stop functioning properly.
Healthy leg veins rely on:
- Calf muscle contraction
- Elastic vein walls
- Competent one-way valves
When valves weaken or fail, blood can flow backwards (a process known as venous reflux). This causes increased pressure inside the vein, leading to:
- Vein enlargement
- Twisting and bulging
- Heaviness and aching
- Skin changes over time
Unlike spider veins, varicose veins typically involve deeper venous insufficiency.
How Are Varicose Veins Assessed?
Varicose veins require a more detailed evaluation. A duplex ultrasound map helps identify insufficiency, vein diameter and flow patterns. This allows the doctor to determine the severity and the most appropriate treatment options.
Ultrasound is the standard method used across Brisbane, the Gold Coast and throughout Australia for diagnosing venous insufficiency.
Treatment Options for Spider Veins
Treatment varies depending on whether spider veins occur alone or alongside deeper issues.
For isolated spider veins, the most common treatment is:
- Microsclerotherapy: A fine-needle technique that targets small surface veins.
Your vein specialist will explain the process, the number of sessions likely needed, and any considerations relating to your health history. Treatment decisions are made on an individual basis after clinical assessment.
Treatment Options for Varicose Veins
For varicose veins, treatment focuses on addressing the source of reflux. Non-surgical options may be recommended depending on the assessment.
These may include techniques such as:
- Endovenous laser treatment (EVLA / EVLT)
- Ultrasound-guided sclerotherapy (UGS)
- Radio Frequency Ablation (RF)
Each method has different considerations depending on your anatomy, symptoms and ultrasound findings. A consultation helps determine what is clinically appropriate.
When Should You See a Vein Specialist?
Signs You Should Book a Vein Assessment
You may consider seeking a medical assessment if you notice:
- Leg heaviness, swelling or aching
- Veins that are bulging, painful or hot to touch
- Skin changes around the ankles
- Increasing clusters of spider veins
- Symptoms worsening after standing
Why Early Evaluation Matters
Early evaluation can help clarify what is happening beneath the surface and prevent progression of venous reflux.


